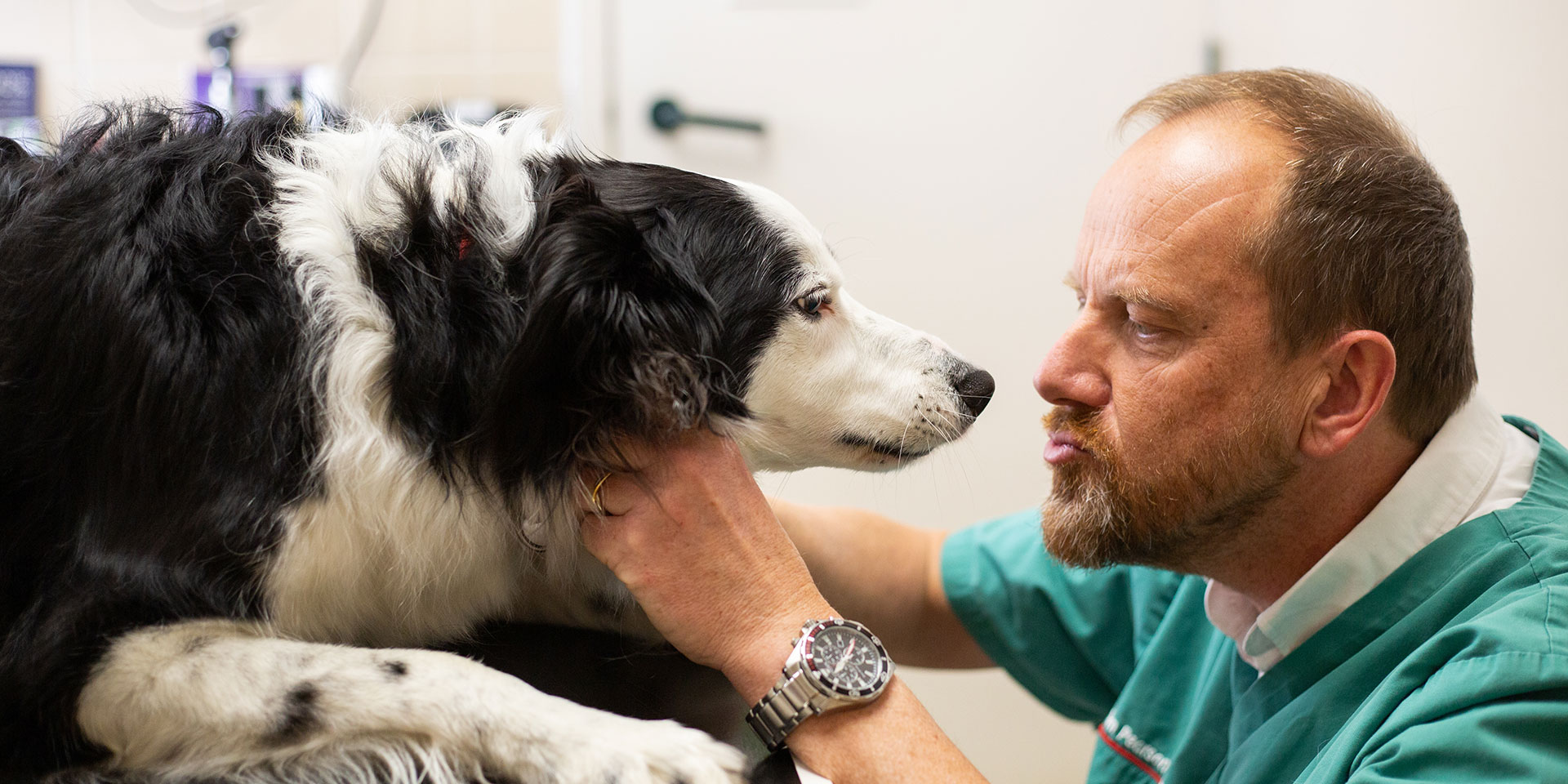
Why choose Orchard House Vets?
We understand that choosing your vet is one of the most important decisions a pet owner can take. Our three Orchard House Veterinary Centres are independent and family owned, and specialise in pets (plus the occasional chicken, owl and wallaby).
Orchard House is the local, community-focused choice. Our clients value our high standards of care for them and their pets. Our staff are highly qualified, caring and approachable. And we care 24 hours a day, 365 days a year – we do not outsource care to a distant emergency centre. Around 9,000 families and households in Tynedale trust us to care for their pets “as if they were our pets”. We hope you will too.
Explore
Our Services
Well Pet Club
At Orchard House we understand that you want to give your pets the best treatment. Our Well Pet Club makes routine healthcare simple and more affordable. A monthly Direct Debit covers annual vaccinations, parasite control, two six-monthly health examinations with a vet, plus discounts on may other products and services.

Book Your Appointment Today
You can now book a routine appointment for your pet at anytime online, whether you are new to the practice or a registered client. For emergencies and operations, please call your local Orchard House Surgery.
Book Now
Our Team
We’re all pet owners at Orchard House. We appreciate the love they give us and, of course, the care they need.